Eighteen months of pandemic-related masking, quarantine, and other public health measures like diligent handwashing not only staved off COVID-19 exposure but kept other more common seasonal illnesses at bay.
During the height of the coronavirus pandemic, flu pretty much disappeared globally. Positive tests for the respiratory syncytial virus (more commonly known as RSV) dropped 97.4% when compared to prior seasonal U.S. averages.
Now that we’ve taken off our masks and have resumed many of our pre-pandemic routines; including returning to our offices, classrooms, and extracurricular activities; there has been a significant uptick in both flu and RSV cases. Young children also likely spent one or two years that are critical for their immune development unexposed to common illnesses due to social distancing.
We now have a “triple pandemic,” if you will, where the community is experiencing outbreaks of COVID, the flu, and RSV, as we loosen mitigation measures, rebuild our immune systems, and gather over the holidays. While these illnesses are not all peaking at the exact same time, there is some concern that their overlap may overwhelm hospitals.
Let’s take a deeper look at what RSV is, how it may present differently from the flu and COVID-19, and when you need to see a doctor.
What is RSV?
Respiratory syncytial virus (RSV) is a cold-like virus that affects the lungs and respiratory system. RSV is highly contagious, spreading through sneezing and coughing, surface contact with droplets, or close contact with an infected person.
According to the American Lung Association, 97% of children have been infected with RSV by the age of two.
Currently, there is no vaccine for RSV. Handwashing with soap and water for at least 20 seconds, staying clear of sick people, and avoiding touching your face with unwashed hands can all help prevent infection.
RSV is generally mild, and can affect people of all ages, however, it is more likely to cause severe illness and hospitalization in infants, young children, or elderly adults, especially people with heart or lung disease or a weakened immune system. In fact, RSV is the leading cause of hospitalization in children under the age of one.
Do I Have RSV,COVID, or Flu?
Unlike the flu, RSV tends to come on gradually, beginning with cold-like symptoms; whereas the flu tends to strike suddenly with a fever. Aches and pains also tend to accompany the flu, however, are not a symptom of RSV.
Early symptoms of RSV may include:
- Runny nose
- Decrease in appetite
- Coughing
- Sneezing
- Fever
- Wheezing
RSV symptoms in infants may be more subtle and include:
- Irritability
- Decreased appetite and activity level
- Trouble breathing, including apnea where there is a pause of more than 10 seconds
This chart from the Children’s National Medical Center will help you understand some of the similarities and differences between these viruses:
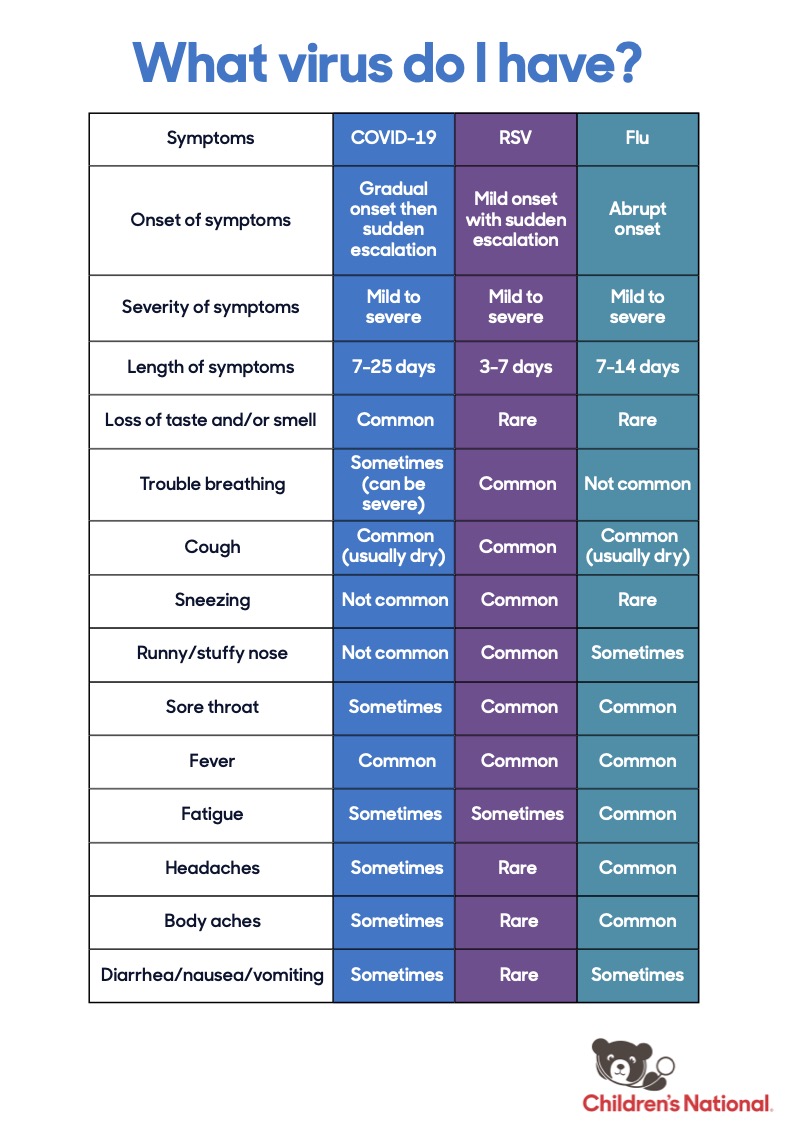
If your symptoms are mild and manageable at home you won’t need to see a doctor. However, only a doctor can confirm whether you have RSV with an oral swab or blood test if necessary.
Treating RSV
People with RSV are typically contagious for three to eight days and most RSV infections will resolve themselves in one to two weeks. Symptoms are managed with over-the-counter pain relievers and fever reducers. Always speak to your child’s physician before administering medication to an infant or small child and never give them aspirin.
It’s important that you stay hydrated if you have RSV. For infants, offer plenty of fluids and look for signs of dehydration including dry mouth, reduced or no urine output, increased fussiness, or sleepiness.
When To See A Physician
If your symptoms are getting worse after 48-72 hours, it may be time to call an ear, nose, and throat specialist.
A barking or wheezing cough could indicate that your infection has spread to the lower respiratory tract which can lead to pneumonia or bronchiolitis, an inflammation of the small airways in the lungs.
You may require hospitalization if your illness becomes severe and you need IV fluids for dehydration or additional oxygen.
There appears to be a connection between RSV and asthma or recurrent wheezing in preschool children. It can also contribute to a worsening of asthma, chronic obstructive pulmonary disease (COPD), or congestive heart failure in adults.
Your Memphis Expert for Ears, Nose, and Throat
If you or your child is experiencing ear, nose, and throat symptoms that won’t go away, Rande Lazar, MD, and the team at ENT Memphis offer appointments at their offices in Memphis and Bartlett.. Many times same-day appointments are available and can be made conveniently online.
Dr. Lazar has decades of expertise in treating both simple and incredibly complex conditions of the ear nose and throat. Make your appointment today.




Comments are closed here.